Investing in health-tech and digitizing healthcare
Health technology is transforming the way we can diagnose, treat and prevent disease, and has the potential to radically improve access to healthcare on a global scale. But technology alone is not the panacea in itself. It is only part of a larger ecosystem of innovators, investors, clinicians, governments, regulators and, of course, patients. To truly capitalize on the potential of healthcare technology; to improve outcomes for patients across the globe, requires new ways of collaborating, new models of service delivery and most crucially, new channels of investment.
It is an interesting juxtaposition. We are living longer, more prosperous lives than ever before, with access to better housing, amenities, employment, education and healthcare facilities, as we become ever more urbanized. By 2050, the World Health Organization (WHO) estimates that two-thirds of the global population will live in urban areas, driven mainly by increasing urbanization in Africa and Asia[1].
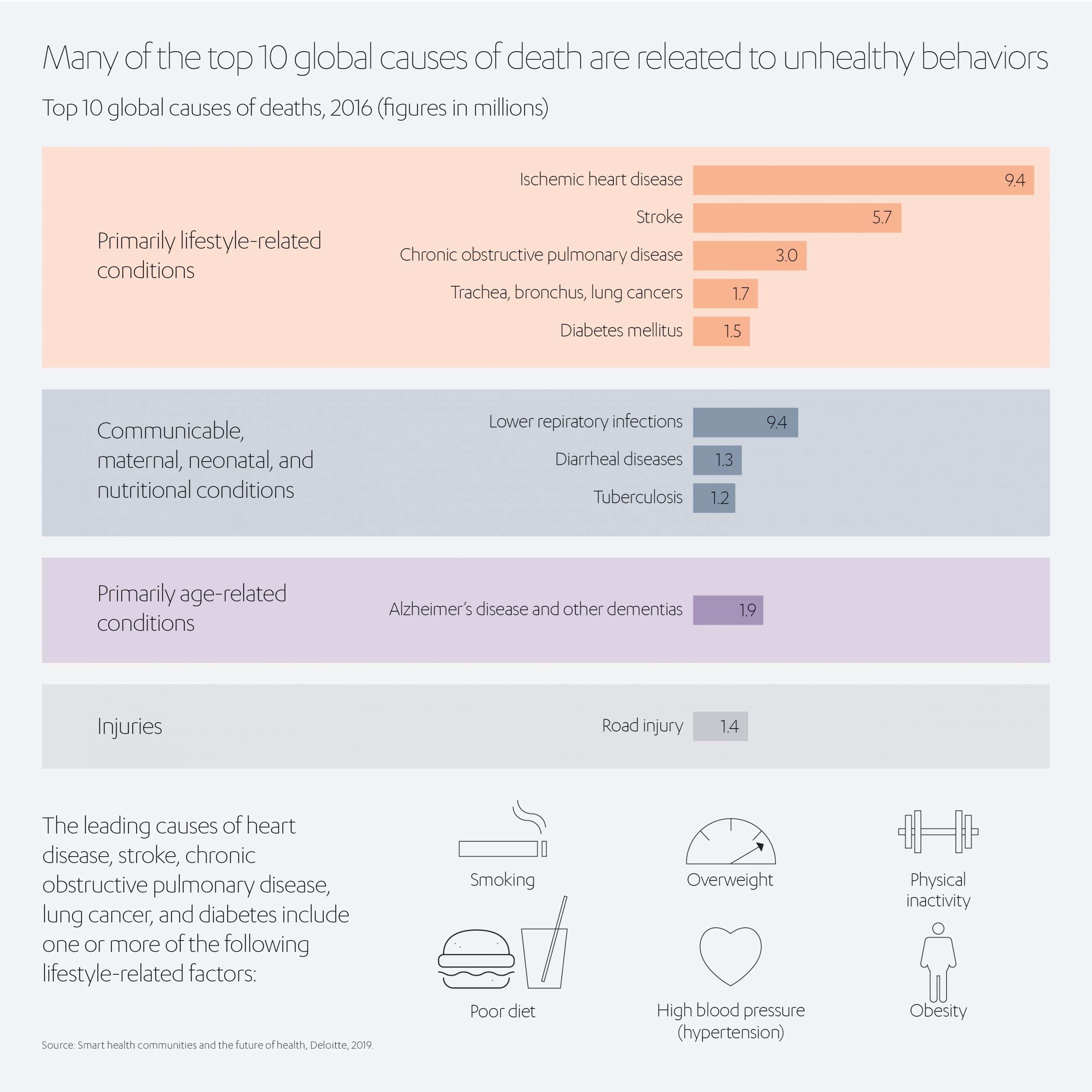
Yet, these are the very factors that are putting more strain on our healthcare services. Our busier, more stressful lifestyles are affecting both our mental and physical health. According to WHO statistics[2], non-communicable diseases, which include diabetes, cancer, heart and lung diseases, are on the rise, accounting for 70% of deaths globally. It attributes the rise to factors such as poor diets, insufficient exercise, smoking, alcohol usage, the growing prevalence of mental health issues, and one of our biggest health threats, air pollution.
In fact, pollution has become the “greatest environmental risk to health”, says a WHO report, affecting nine out of ten people and killing an annual seven million people prematurely through non-communicable diseases. Between 2030 and 2050, climate change will lead to an additional 250,000 deaths every year, not just through pollution but also heat stress, diarrhea, malaria and malnutrition in the World’s poorest countries[3].
All these elements combined are putting increasing pressure on our healthcare systems, with rising treatment costs and burgeoning time pressure on medical establishments and clinicians.
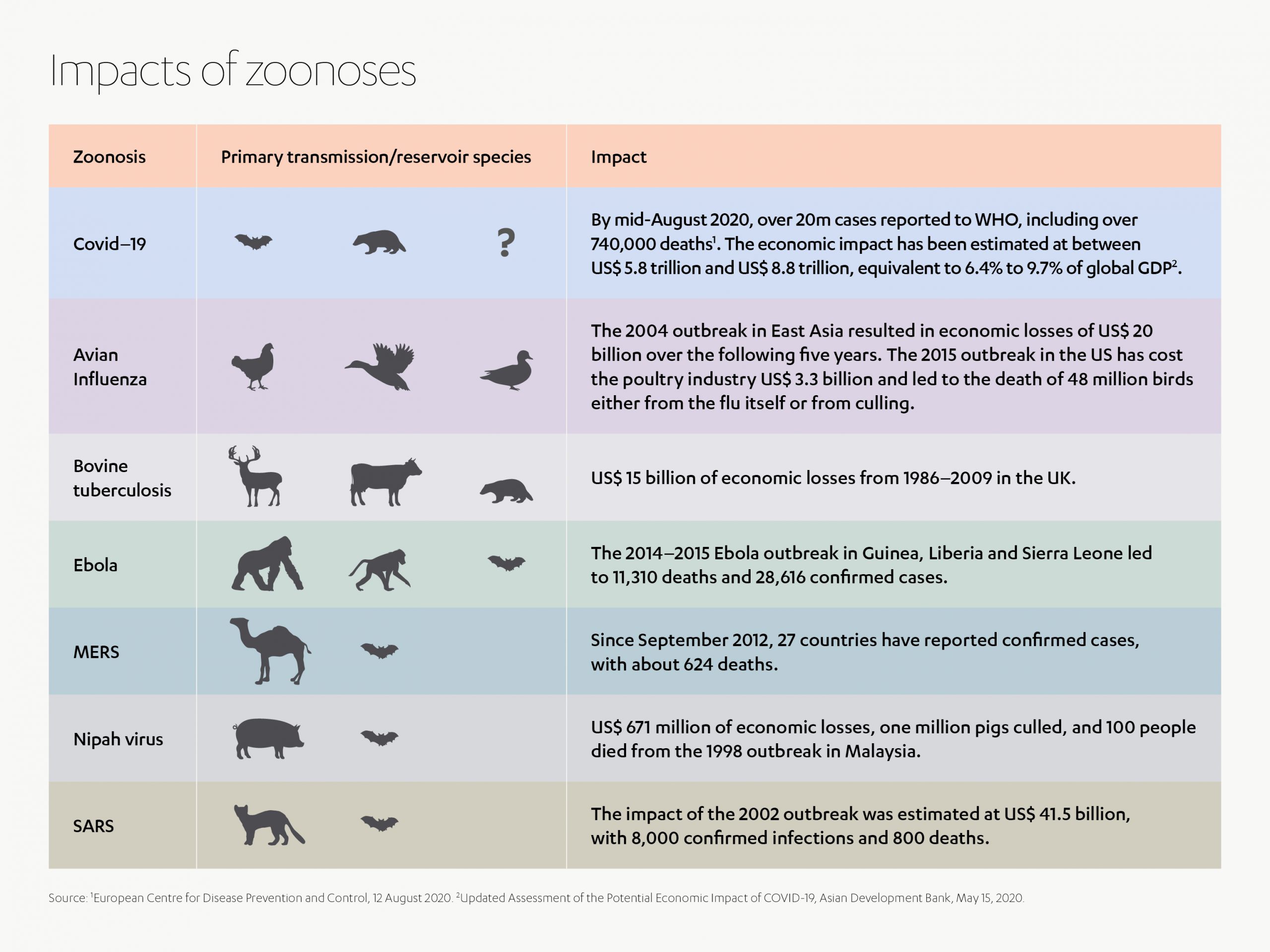
Cramming more and more people into towns and cities where healthcare infrastructures are already creaking also has an indirect impact on healthcare risks, not least of which is rise of ‘zoonotic’ diseases – diseases which pass from animals to humans. Fresh in our minds, COVID-19, which continues to contribute to thousands of deaths worldwide, is itself, a zoonotic disease, and although the most recent and most devastating example, it is a far from an unusual case. According to the National Institute of Health, zoonotic diseases account for 60% of known infectious diseases and 75% of emerging contagions. Notable examples include Ebola, bird flu (H5N1) and the world’s biggest killer – malaria, which affects 500 million people and kills 2.7 million every year[4].
Health technology – the new game changer
The on-going battle against both communicable and non-communicable diseases, with few notable successes, demonstrates our patchy track record in stemming the tide of such global health threats. However, artificial intelligence (AI) driven advances in healthcare technology could be about to herald a new era in the fight against illness and disease, opening up new pathways to access high quality healthcare for those that most need it.
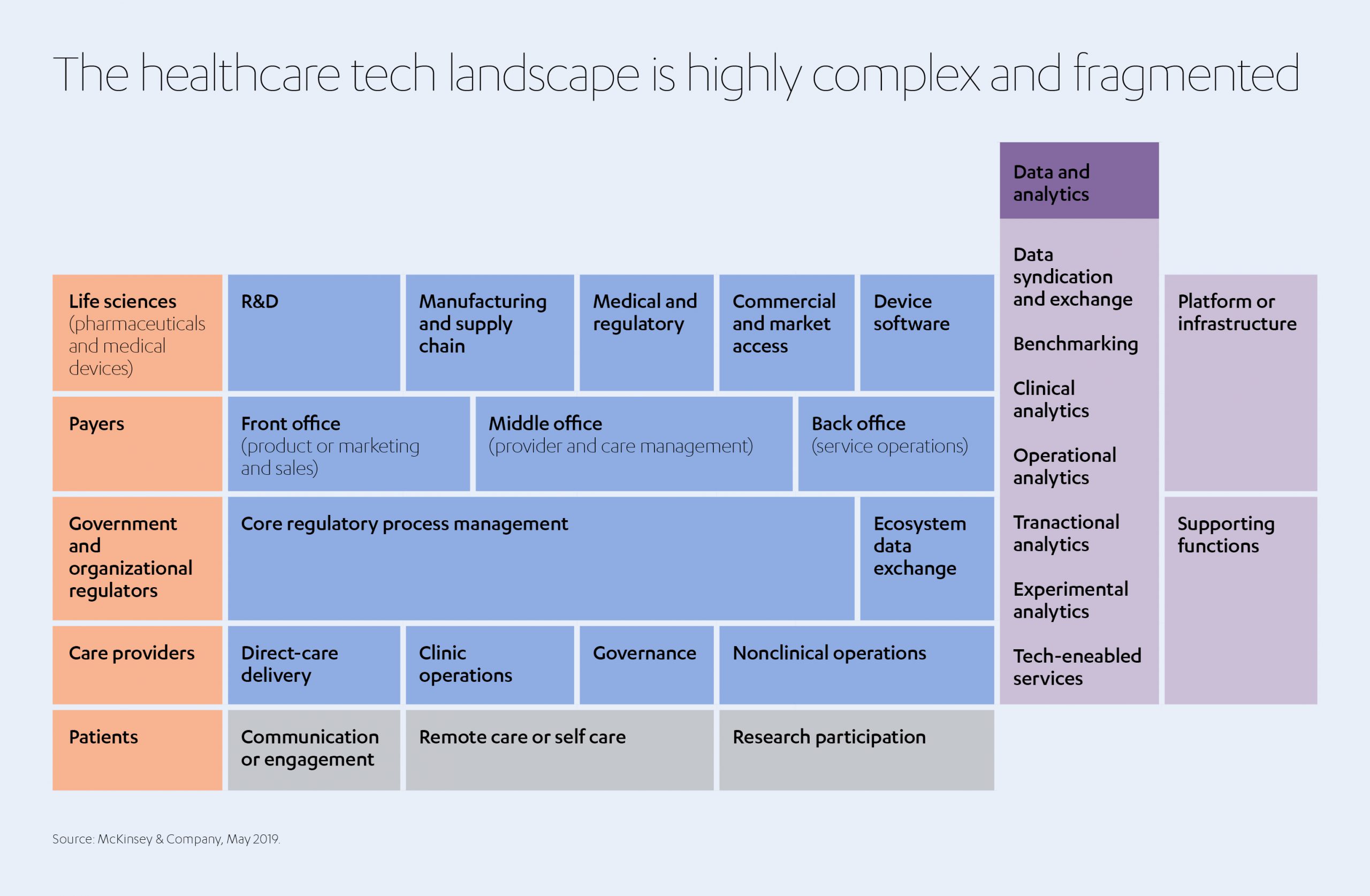
The WHO defines ‘health technology’ as the “application of organized knowledge and skills in the form of devices, medicines, vaccines, procedures and systems developed to solve a health problem and improve quality of lives.”[5] In other words, it involves a highly complex combination of different stakeholders and regulatory factors which, suggests global consulting firm McKinsey & Company, is perhaps why the healthcare industry currently falls behind other sectors in the pace of digital transformation.
Leading the way are AI and machine learning, which can turn vast amounts of patient health data into refined insights for treating, preventing and even predicting diseases[6]. Programmed with a complex set of ‘what-if’ rules-based scenarios, AI can collate and organize global health data at a speed that was previously impossible. Through the results that emerge, clinicians can come to understand recurring patterns and develop treatment models based on specific patient attributes[7].
There are already numerous relatively simple examples of how AI is being applied within the health industry.

A smartwatch produced by Empatica and approved by the US Food and Drug Administration (FDA), for example, uses AI algorithms to measure temperature data and alert the wearer of infection before any symptoms are felt, which could potentially help in detecting early-stage viruses like COVID-19[8].
IBM’s Watson Health system combines human expertise with augmented intelligence to help health professionals and researchers build their knowledge and provide better care across hundreds of hospitals globally[9].
For diabetes sufferers, for example, Watson Health can predict alterations in glucose levels up to three hours in advance of the onset. And in the oncology field, its intelligent systems can analyze tens of millions of data points in just seconds and identify 300 alternative therapies for at least 12 cancer types, accounting for 80% of the global cancer incidences[10].
Google’s DeepMind AI platform is also supporting clinicians in providing improved patient outcomes[11]. It has developed a technology for the early diagnosis of acute kidney injury which affects one in five hospital patients in the UK and US. In the UK alone, the condition costs hospitals more than US$ 1.2 billion every year[12].
Another area where AI is already making a difference is in improving care for the elderly, where robots are being used to converse and socially interact with patients. Long periods in hospitals and care homes can be isolating, particularly for older patients. Robotic interaction helps them remain independent for longer and reduces the need for hospitalization and care homes. This enhances their quality of life, helps to keep their minds sharp, and relieves the economic burden of healthcare systems within aging populations[13].
Economics and personal health monitoring
The motivations for AI-driven healthcare lie as much in government economics as patient outcomes. In fact, the two are inextricable, as rising health issues place their own burden on government funds. Forbes estimates that by 2026, AI could yield annual savings of US$ 150 billion within the health sector and eventually address 20% of unmet clinical demand. By 2021, AI investment is expected to reach US$ 6.6 billion.
The UK government alone has invested around US$ 306 million in a ‘National Artificial Intelligence Lab’ (NHSX) to digitize its National Health Service (NHS). It is aimed at reducing 30 million outpatient appointments, saving more than US$ 1.2 billion that can be reinvested in front line care, and saving patients what is describes as unnecessary hospital journeys[14].
AI-driven wearable technology is seen as another way of significantly reducing hospital visits and the growing time burden faced by clinicians.[15] Allowing users to monitor their own health, exercise levels and sleep patterns, they can ultimately take a preventative rather than treatment approach to healthcare. On a broader scale, wearables give medical insurance companies a barometer through which they can now offer personalized cost packages to their customers, and incentives which will potentially lead to the behavioral change of policy holders[16]. Wearables also offer employers a way to vastly improve their productivity (lost work time through sickness can cost economies billions of dollars)[17].
Research by Business Insider magazine in the US found that more than 80% of consumers are open to using a wearable. From the original fitness tracking devices that link up to smartphone apps, wearables have progressed into smart health watches that measure heart rhythms, ECG monitors that can measure an electrocardiogram and detect atrial fibrillation (irregular heartbeat and breath), and blood pressure monitors that can store, track and share data with physicians, gain insights into the wearer’s personal habits and trigger behavioral change.
Research suggests that the health and fitness wearables market will continue to grow. Over the past four years, the market has more than tripled in the US alone and is predicted grow at an annual 10% to surpass 120 million users by 2023[18]. This represents more than a third of the country’s 330 million population.

Along with wearables, another trend is towards developing smaller devices to make diagnostics more available and accessible. One example is a handheld device which uses 9,000 sensors to perform ultrasound procedures – without the harmful radiation implications associated with traditional ultrasound machines. It is also thought to be a way of providing affordable diagnosis to the two-thirds of the world’s population with no access to ultrasound technology [19].
Leveraging the latest advances in AI technology to increase the availability and accessibility of effective diagnostic devices is a priority for healthcare providers, governments and NGOs, for both infectious and non-infectious conditions. Diagnostics influence around 70% of healthcare decisions, yet diagnostic tests currently make up only 3% to 5% of healthcare spending[20]. Improving access to blood glucose measurements, for example, could help to improve diabetes detection among the 50% of people in low- and middle-income countries who do not know they have it, giving millions the chance of better treatment and improved long-term outcomes.
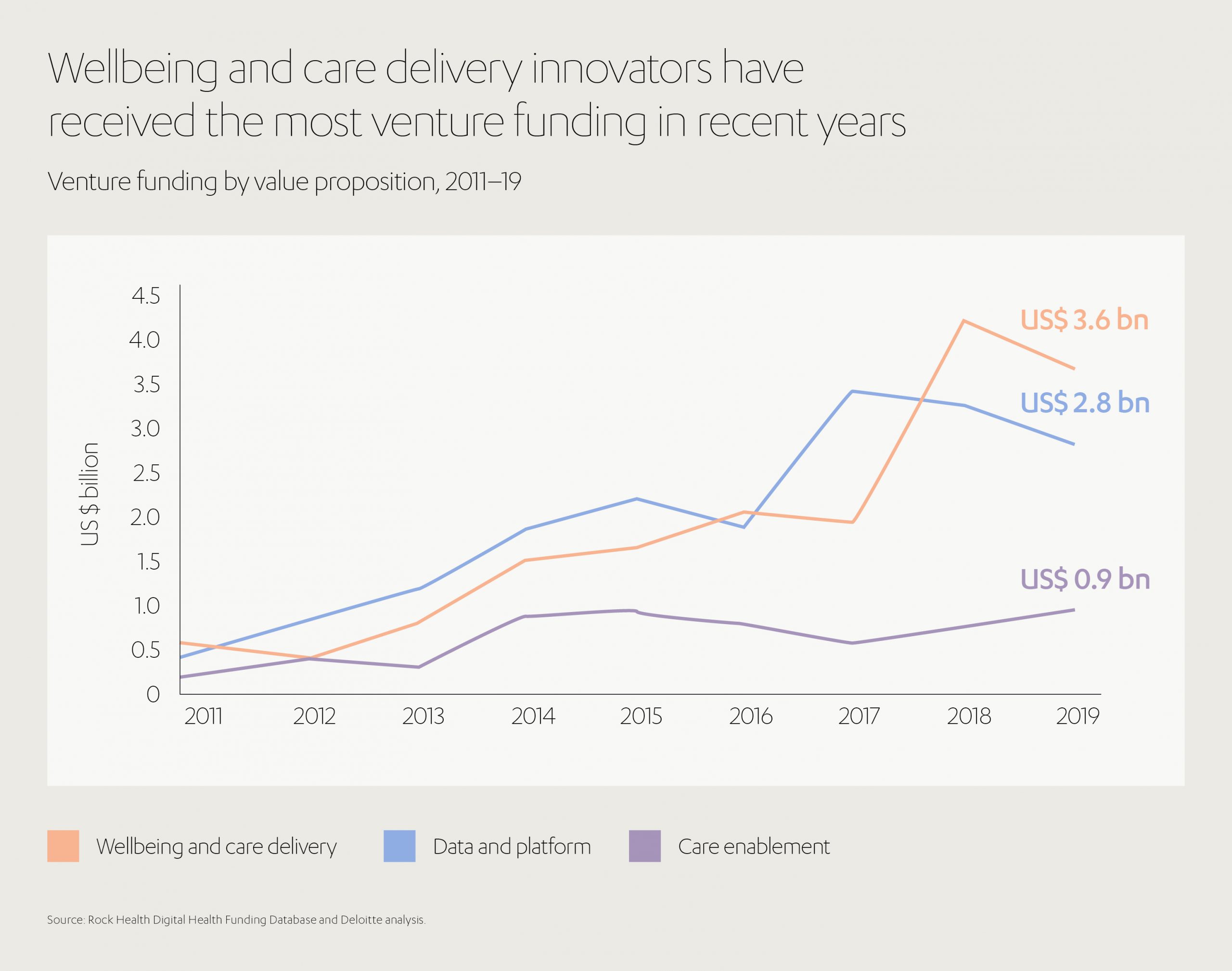
For private investors, the current pace of innovation in healthcare technology promises the opportunity to capture real growth value. Google and Apple are two of the most well knownamong a plethora of companies that have invested in some of the latest wearable innovations. According to Forbes, 2019 saw billions of dollars invested into more than 100 digital health companies[21]. Notable examples include Google’s acquisition of fitness tracking wearable, Fitbit, and Amazon’s purchase of Health Navigator, which uses big data analytical techniques to provide health coaching[22]. Healthcare giant Optum has also expanded its offering of patient self-monitoring devices by acquiring Vivify Health, a cloud-based platform through which clinicians can provide remote care[23].
Virtual health
Equally, the possibilities of virtual health are expanding – where patients and clinicians can have ‘virtual’ consultations, in real-time, and from almost any location. In the US, virtual health or ‘telemedicine’ services are forecast to increase 16.8% between 2017 and 2023[24].
Through virtual health, clinicians can provide care and support at the time and location that best suits the patient – particularly where there are physical challenges in distance and accessibility to healthcare provision[25]. The potential of virtual health is further driven by the data individual patients can collect and share with their clinicians through wearable technologies.
Clinical virtual health trials are already taking place all over the world, with participants never needing to leave their homes. Researchers from the Stanford University School of Medicine studied 400,000 people on how smart watches can safely identify ‘atrial fibrillation’ heart rate irregularities. Around 33 million people worldwide have the condition and up to 30% of cases go undiagnosed until life-threatening complications arise[26]. In the study, 80% of participants who received irregular pulse notifications through their smart watch were found to have atrial fibrillation. Of these, 57% sought medical attention[27].
Investing in possibilities
The Jameel family have long recognized the need to invest in healthcare as one of the key building blocks of the infrastructure of life. Indeed, the late founder of today’s diversified businesses and global family philanthropy was a founding member of a number of health-oriented initiatives in Saudi Arabia and across the region, including the Abdul Latif Jameel Hospital for Medical Rehabilitation, established in 1995, the first non-profit rehabilitation hospital in Saudi Arabia, providing comprehensive care for adults and children.
In 2018, the Abdul Latif Jameel Clinic for Machine Learning in Health, or ‘Jameel Clinic’ (J-Clinic), based at Massachusetts Institute of Technology (MIT) was co-founded by Community Jameel, and – as part of its mission – is today at the forefront of research into healthcare technology, with a focus on using AI to model biological data across modalities such as imaging, text and genomics, and making new discoveries in machine learning, biology, chemistry and clinical sciences[28].
Within the context of the current pandemic, for example, Jameel Clinic researchers successfully used AI to produce data-driven models to yield accurate predictions of how infection rates evolve, based on peoples’ movement patterns and congregation behaviors[29].
The Jameel Clinic also conducted a study to ‘predict’ if an individual was over-tired, rundown or stressed, thereby increasing their likelihood of falling ill, based on data collected from wearable sensors and smartwatches[30]. The team plan to roll-out their research to look at viral infections, such as SARS-CoV-2, the virus that causes COVID-19[31].
In February 2020, another spectacular success for Jameel Clinic was the AI-based identification of a powerful new antibiotic compound, Halcin. The molecule picked out by the model – screened from more than a hundred million chemical compounds in a matter of days – was predicted to have strong antibacterial activity and a chemical structure different from any existing antibiotics. Using a different machine-learning model, the researchers also showed that this molecule would likely have low toxicity to human cells.
Another Community Jameel co-founded lab, the Abdul Latif Jameel Institute for Disease and Emergency Analytics, or ‘Jameel Institute’ (J-IDEA) based at Imperial College London, is using data analytics to identify, map and prioritize preventable communicable disease risk and public health worldwide[32].
Out of the lab, into the community
It’s not only a question of investing in R&D to develop new innovations and technologies, however. To make a lasting, sustainable improvement in healthcare means getting the technology out of the labs and out into the field to address the issues of access to healthcare and health-tech in the World’s developing regions where it is sorely needed. That’s why Abdul Latif Jameel is also partnering with leading health tech companies across the globe, with the aim of strengthening healthcare accessibility.
In 2017, it partnered with Japanese health tech innovators Cyberdyne, which specializes in pioneering spinal injury rehabilitation technology using robotic exoskeletons, in a first to bring this cutting edge technology to Saudi Arabia. The partnership was extended in 2019, with the aim of rolling out Cyberdyne’s Hybrid Assistive Limb (HAL®) technology across the Gulf region[33] and establishing the Abdul Latif Jameel Hospital as a regional training center.
 It has established a similar partnership with another Japanese health tech pioneer, Cellspect, to provide speedy and affordable blood testing in developing countries across the Middle East, Africa, Southeast Asia and India.
It has established a similar partnership with another Japanese health tech pioneer, Cellspect, to provide speedy and affordable blood testing in developing countries across the Middle East, Africa, Southeast Asia and India.
Cellspect’s Point of Care Testing device currently checks sugar metabolism, lipid and liver function – delivering results in just five minutes.
And with the aim to help commercialize and distribute cutting edge technologies, Abdul Latif Jameel also partnered with the Japanese Organization for Medical Device Development (JOMDD) to help scientists, engineers, clinicians and entrepreneurs push forward new devices and technology.
Emerging technologies have the potential to help patients in other ways, too. 3D printing is increasingly being used to create dentures and customized casts for broken bones[34]. One of the most significant breakthroughs has been in creating 3D-printed ‘prosthetic’ artificial limbs for amputees. Traditionally costing tens of thousands of dollars, prosthetics have been only available to the comparative few. Now, sophisticated 3D prosthetics can be made for less than US$ 30 and are being offered to patients from some of the world’s poorest countries[35].
The onset of 5G broadband will expand the possibilities of health technology still further, with vastly faster connection speeds enabling for the transfer and streaming of big data (large and complex data sets) in a way that previously has not been possible. 5G also opens up the possibility for surgeons to perform procedures from other continents aided by robotic technologies.[36] With a latency lag of just 0.1 seconds, surgeons could potentially conduct live operations on the other side of the world using IOT-connected robotic technologies[37].
Securing our data
In addition to the many technological and financial challenges involved in fully realizing the potential of technology to revolutionize healthcare as we know it, another major hurdle is data security. The prospect of creating collaborative data banks across both hospitals and geographic territories shows huge potential for gaining broader learning. But in a sector that is founded on the principle of patient confidentiality, there are some significant pros and cons to balance. Even anonymized personal information passed to a clinic could include sensitive information on the patient’s past addresses, lifestyle and family relationships[38].
Having the right cross-border regulatory measures in place to ensure sensitive data is not compromised under any circumstances will be paramount. But with the proliferation of personal information already available across the internet, there is no easy solution to protecting shared medical information.
As the health technology market becomes more competitive, so too will the goalposts for success become tougher for both incumbents and new entrants. To lead the pack, suggests McKinsey, the core offerings of health technology developers will need to earn the regard of investors by understanding customer perceptions, conducting sound due diligence, building solid technological frameworks and delivering a demonstrable impact on those their innovations serve.
They must also be ready and able to upscale, based on the demand their innovations create, and have a clear road map for further research and development as demand dynamics change over time[39].
The health technology market has suddenly found itself riding of the crest of a wave.
Moving forward, momentum and continued innovation will be key, along with new channels of finance from investors with a long-term commitment and a holistic vision – such as Abdul Latif Jameel – that define success not only in terms of financial returns, but also humanitarian outcomes.
[1] https://cities-spotlight.who.int/
[2] https://www.who.int/news-room/feature-stories/ten-threats-to-global-health-in-2019
[3] https://www.who.int/news-room/feature-stories/ten-threats-to-global-health-in-2019
[4] https://www.who.int/whr/1996/media_centre/executive_summary1/en/index9.html
[5] https://www.who.int/health-technology-assessment/about/healthtechnology/en/
[6] https://www.telegraph.co.uk/business/open-economy/new-technologies-transforming-healthcare/
[7] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6616181/
[8] https://www.jclinic.mit.edu/post/ml-for-covid-19-can-ai-give-you-an-alert-indicating-a-viral-infection-before-you-feel-symptoms
[9] https://www.ibm.com/watson-health/about/get-the-facts
[10] https://www.healthcareglobal.com/technology/four-ways-which-watson-transforming-healthcare-sector
[11] https://deepmind.com/blog/announcements/deepmind-health-joins-google-health
[12] https://deepmind.com/blog/article/predicting-patient-deterioration
[13] https://www.pwc.com/gx/en/industries/healthcare/publications/ai-robotics-new-health/transforming-healthcare.html
[14] https://www.england.nhs.uk/2019/06/nhs-aims-to-be-a-world-leader-in-ai-and-machine-learning-within-5-years/
[15] https://www.businessinsider.com/wearable-technology-healthcare-medical-devices?r=US&IR=T
[16] https://www.forbes.com/sites/reenitadas/2019/02/04/the-top-five-digital-health-technologies-in-2019/#4f4e55766c0f
[17] https://www.forbes.com/sites/ashleystahl/2020/03/12/3-ways-coronavirus-may-impact-the-future-of-the-workforce/#744b8bf1cef5
[18] https://www.businessinsider.com/wearable-technology-healthcare-medical-devices?r=US&IR=T
[19] https://www2.deloitte.com/us/en/insights/industry/health-care/health-tech-investment-trends.html
[20] https://stm.sciencemag.org/content/6/226/226ed6
[21] https://www.forbes.com/sites/greglicholai/2020/01/14/digital-healthcare-growth-drivers-in-2020/#74a8bfdb511d
[22] https://www.forbes.com/sites/greglicholai/2020/01/14/digital-healthcare-growth-drivers-in-2020/#74a8bfdb511d
[23] https://hitconsultant.net/2019/11/01/unitedhealth-optum-acquires-vivify-health/
[24] https://telemedicine.arizona.edu/blog/7-telemedicine-concerns-and-how-overcome-them
[25] https://www2.deloitte.com/content/dam/insights/us/articles/GLOB22843-Global-HC-Outlook/DI-Global-HC-Outlook-Report.pdf
[26] https://eu.usatoday.com/story/tech/2020/02/25/apple-watch-johnson-johnson-study-to-reduce-stroke-risk/4866152002/
[27] http://med.stanford.edu/news/all-news/2019/03/apple-heart-study-demonstrates-ability-of-wearable-technology.html
[28] https://www.jclinic.mit.edu/
[29] https://www.jclinic.mit.edu/post/neural-network-aided-quarantine-control-model-estimation-of-covid-spread
[30] https://www.jclinic.mit.edu/post/ml-for-covid-19-can-ai-give-you-an-alert-indicating-a-viral-infection-before-you-feel-symptoms
[31] https://www.jclinic.mit.edu/post/ml-for-covid-19-can-ai-give-you-an-alert-indicating-a-viral-infection-before-you-feel-symptoms
[32] https://www.imperial.ac.uk/jameel-institute/research/strengthening-health-systems/
[33] https://www.alj.com/en/news/abdul-latif-jameel-and-cyberdyne-expand-collaboration-across-gcc-region/
[34] https://www.healthecareers.com/article/healthcare-news/medical-technology
[35] https://www.huffingtonpost.co.uk/entry/these-low-cost-3d-printed-prosthetics-are-giving-people-a-hand_n_5b506664e4b086f60991a0cd?ri18n=true
[36] https://www.telegraph.co.uk/business/open-economy/new-technologies-transforming-healthcare/
[37] https://www.independent.co.uk/life-style/gadgets-and-tech/news/5g-surgery-china-robotic-operation-a8732861.html
[38] https://www.theguardian.com/commentisfree/2020/feb/16/our-personal-health-history-is-too-valuable-to-be-harvested-by-tech-giants
[39] https://www.mckinsey.com/industries/private-equity-and-principal-investors/our-insights/private-equity-opportunities-in-healthcare-tech





 1x
1x

 Added to press kit
Added to press kit


